If you’re building a care navigation, care routing, or digital front door experience, provider data accuracy isn’t optional—it’s foundational. Yet across the healthcare industry, many platforms are still guiding members using provider directories that don’t reflect real-world access.
A recent blog post from Zocdoc, “Ghost Networks Explained: Why Healthcare Provider Directories Fail,” clearly outlines the problem. Ghost networks occur when provider directories list doctors or facilities as in-network even though they aren’t realistically available—because they’ve moved, stopped accepting new patients, changed network participation, or are simply unreachable. The result is a directory that looks complete but fails members at the moment they try to act on it.
This isn’t a fringe issue. It’s systemic—and it’s breaking care navigation.
How Common Are Ghost Networks?
Ghost networks are far more prevalent than many platforms realize. According to audits cited by Zocdoc, 45–52% of Medicare Advantage provider listings contain at least one inaccuracy, such as an incorrect address, phone number, or network status. In a U.S. Senate Finance Committee secret shopper study focused on mental health access, patients were able to successfully book an appointment only 18% of the time, largely due to inaccurate directory information.
For care navigation and routing platforms, these numbers translate directly into:
- Members routed to dead ends
- Delays in care
- Increased abandonment and frustration
- Higher support costs and erosion of trust
Ghost networks don’t just degrade user experience—they undermine the core promise of guiding members to care.
Why Ghost Networks Break Care Navigation and Care Routing
Care navigation depends on actionable accuracy. It’s not enough to show that a provider is technically in-network. Members need confidence that:
- The provider actually practices at the listed location
- The plan truly covers them
- The recommended route leads to real, accessible care
Ghost networks introduce false destinations into routing logic. Navigation flows may look correct, but members are forced to validate everything themselves—calling offices, rechecking coverage, and starting over when reality doesn’t match the directory.
As the Zocdoc post makes clear, this is less a UX issue and more a failure of access pathways. When directories aren’t trustworthy, navigation becomes trial-and-error instead of guidance.
What Solving Ghost Networks Actually Requires
Addressing ghost networks at an industry level requires better infrastructure—not just better interfaces. Specifically, platforms need:
- Provider directory data delivered in a single, normalized format
- Frequent refresh cycles that reflect how often provider data changes
- Confidence signals to distinguish reliable listings from risky ones
- Feedback loops that correct inaccuracies at the source, not just downstream
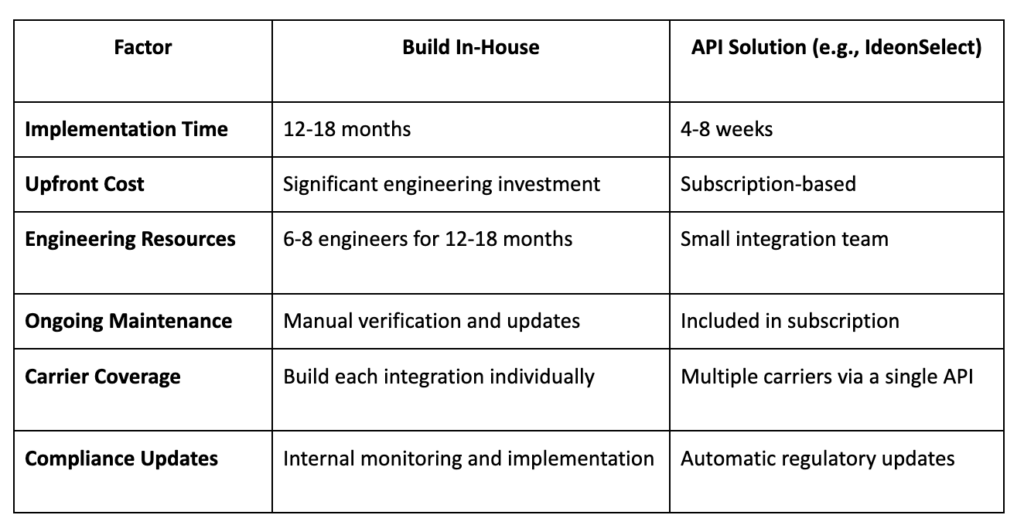
This is where API-first provider data and carrier relationships become critical.
How Ideon Helps Solve Ghost Networks at the Source
IdeonSelect provides provider directory data purpose-built for care navigation, care routing, digital front doors, and digital health platforms. Instead of trying to “patch” directory issues downstream in UX, Ideon focuses on the infrastructure that prevents bad listings from becoming routed destinations in the first place.
In practical terms, here’s what happens in your navigation experience when it’s powered by Ideon’s API:
- Ingest normalized, accurate provider directory data that’s mapped at the carrier, network, plan, and provider levels.
- Use built-in location accuracy signals to reduce risky results
- Benefit from Ideon’s upstream data quality checks so issues don’t keep reappearing
One API for Normalized Provider Directory Data
IdeonSelect delivers provider directory data from every carrier nationwide through a single API, in one consistent schema. Instead of stitching together dozens of carrier-specific files, platforms receive a unified feed that includes:
- Provider specialties and subspecialties
- Locations and contact details
- Network participation by plan
This makes it far easier to build reliable care navigation and routing logic without reconciling conflicting data sources.
Direct Carrier Relationships, Plus Rigorous QA
Ghost networks persist when inaccuracies are never corrected upstream. Ideon addresses this through a combination of:
- Direct relationships with carriers, providing authoritative network data at scale
- A rigorous QA process that evaluates provider directory data across multiple sources to detect inconsistencies
When issues are identified—such as incorrect network participation or stale locations—Ideon works directly with carriers to correct data at the source, preventing errors from propagating across the ecosystem.
Continuously Refreshed Data and Network‑Scale Coverage
Ideon’s provider directory API covers 8.5 million providers and more than 5,000 networks nationwide, spanning individual, group, Medicare Advantage, and Medicaid markets. Data is refreshed on an ongoing basis—multiple times per month on average—so platforms aren’t routing members based on stale snapshots.
This combination of scale, refresh cadence, and source-level correction helps platforms maintain healthier networks over time, not just cleaner search results.
Address Confidence Scores
One of the most common ghost-network failures is routing members to the wrong location. Ideon’s Address Confidence Scores assign a High, Medium, or Low confidence rating to every provider address using machine learning and verified data.
Platforms can use these scores to:
- Filter or deprioritize low-confidence locations
- Reduce misroutes and failed appointments
- Build smarter routing logic without pretending the data is perfect
From Directory Accuracy to Real Access
As the Zocdoc post underscores, access isn’t real unless it can be acted on. For care navigation and care routing platforms, success shouldn’t be measured by how many providers appear in a directory—but by how often members actually reach appropriate, in-network care without friction.
Ghost networks are a systemic industry problem. But with normalized provider directory data, strong carrier relationships, rigorous QA, and continuous correction at the source, platforms can stop routing members to dead ends.
If you’re building or improving a platform with care navigation or provider search functionality, consider the following:
- Do we receive directory data in a single normalized format?
- How often is it refreshed?
- Do we constantly experience data quality issues around provider locations and in-network status?
- When we find inaccuracies, can they be corrected upstream—or do they keep reappearing in the next refresh?
Explore Ideon for Care Navigation and Digital Health
If you’re building care navigation, care routing, or a digital front door, IdeonSelect can help you reduce “false destinations” with normalized provider directory data delivered through a single API.