What Is Provider Data Management in Healthcare? A Complete Guide for 2026
Published on February 12, 2026
By: Ideon

Provider data management (PDM) is the foundational infrastructure determining whether patients find accurate provider information, whether claims process correctly, and whether organizations meet regulatory compliance. With 62% of members demanding precise provider data and CMS enforcement tightening through 2027, organizations face a strategic decision: spend 12-18 months building complex PDM infrastructure internally, or leverage API-driven solutions to launch in weeks with automatic compliance.
Healthcare consumers are making decisions with their feet. Over 33% of members will switch health plans for better digital capabilities and provider data access. This shift has transformed provider data management from back-office administrative function to competitive differentiator—the invisible infrastructure determining member satisfaction, regulatory standing, and operational efficiency.
The challenge is clear: provider information changes constantly, with inaccuracies persisting an average of 540 days in systems without automated verification. Meanwhile, regulatory requirements have accelerated dramatically. Medicare Advantage plans must verify directories every 90 days. The No Surprises Act demands 1-business-day response times. Medicaid programs require 30-day updates as of July 2025.
For benefits technology platforms, health plans, and TPAs, provider data management represents a fork in the road. Build complex infrastructure internally—requiring 12-18 months and significant engineering resources—or integrate API-driven solutions delivering accuracy, compliance, and scalability in weeks rather than months.
I. What Is Provider Data Management
Provider data management (PDM) is the systematic process of collecting, organizing, maintaining, and updating healthcare provider information across organizations. This data layer powers the provider directories patients use to find care, enables claims processing accuracy, and provides required infrastructure for regulatory compliance with CMS, state agencies, and federal mandates.
What PDM encompasses:
- Provider credentials: NPI numbers, medical licenses, board certifications, DEA registrations
- Practice information: Office locations, contact details, languages spoken, office hours
- Network affiliations: Plan participation status, network tiers, panel capacity
- Clinical capabilities: Hospital privileges, specialties, subspecialties, telehealth availability
- Billing details: Tax IDs, group affiliations, claims submission requirements
Multiple stakeholders depend on effective PDM: health insurance carriers (Medicare Advantage, commercial plans, Medicaid programs), benefits technology platforms (HR tech vendors, ICHRA administrators, broker platforms), healthcare systems (hospitals, physician groups, integrated delivery networks), and third-party administrators.
The modern challenge is significant. Without automation, provider data inaccuracies persist an average of 540 days—creating compliance exposure, member frustration, and operational inefficiency. Organizations face a strategic choice: build complex PDM infrastructure in-house or leverage API-driven solutions that handle the data plumbing.
II. Why Provider Data Management Matters in 2025
For Patients and Members
Member expectations have fundamentally shifted. 62% of members now seek more precise provider information to make informed care decisions. Among younger demographics, demand is even more pronounced: 70% of Millennials and 64% of Gen Z want comprehensive provider details including locations, availability, and network status before selecting care.
The business impact is direct. Over 33% of members indicate willingness to switch health plans for better data access and digital capabilities. Inaccurate directories create tangible harm: delayed care, wrong provider visits, and surprise bills that erode member trust and drive churn.
For Health Plans and Payers
Regulatory compliance has become increasingly enforcement-focused. Medicare Advantage plans must verify and update provider directories every 90 days. The No Surprises Act requires response to provider inquiries within 1 business day. Medicaid programs mandate 30-day updates as of July 1, 2025. Non-compliance triggers penalties and audit exposure that compounds over time.
For Operations and Efficiency
Accurate provider data reduces claims denials and payment delays. Streamlined credentialing and network management translate directly to operational cost reduction. Organizations with centralized, accurate PDM systems report ROI of $753-$1,982 per attained enrollee through improved data quality—a measurable return on infrastructure investment.
III. Core Components of Provider Data Management Systems
Effective PDM systems integrate six interconnected components that work together to maintain accurate, compliant provider information.
Data Collection and Aggregation gathers provider information from multiple sources: initial credentialing applications, primary source verification (medical boards, DEA, NPPES), electronic health records, carrier enrollment forms, and claims systems. The challenge is that each source uses different formats, taxonomies, and identifiers—creating fragmentation that compounds over time.
Data Storage and Centralization creates a single source of truth for provider information. Cloud-based platforms provide accessibility across organizations while maintaining security and audit capabilities. Centralized repositories ensure updates propagate to all downstream systems simultaneously.
Data Normalization and Standardization converts disparate formats into unified schema. This includes mapping specialty taxonomies (NUCC codes, custom classifications), standardizing addresses and phone numbers, and resolving duplicate records and conflicting information.
Data Validation and Verification automates credential verification against primary sources, replacing manual phone calls and mail surveys. Network status validation with carriers confirms participation. Practice location confirmation verifies addresses and hours.
Data Distribution and Access flows verified data to provider directories (web, mobile, print), API endpoints for real-time search, care coordination systems, and claims processing platforms through real-time channels rather than batch transfers.
Data Governance and Quality Control establishes accountability, defines quality metrics, and maintains audit trails for compliance reporting readiness.
IV. Key Challenges in Healthcare PDM
Data Fragmentation Across Systems scatters provider information across disconnected platforms—EHR, billing, credentialing, claims—with no single source of truth. Each system holds partial information, and inconsistencies compound as data ages.
Manual Processes and Labor Intensity consume significant staff resources. Provider offices field data requests from dozens of health plans, each with different forms and timelines. Manual verification cycles are time-consuming and error-prone: phone calls go unanswered, faxes disappear, surveys are ignored.
Persistent Directory Inaccuracies including wrong addresses, outdated affiliations, and incorrect network status remain uncorrected for an average of 540 days without automated verification—well beyond regulatory compliance windows and long enough to frustrate members seeking care.
Regulatory Compliance Complexity creates overlapping requirements: Medicare Advantage 90-day verification cycles, No Surprises Act 1-business-day responses, Medicaid 30-day updates (effective July 2025), and the CMS Plan Finder mandate requiring MA plans to publish directories by 2027. Multi-state variations add another layer.
Real-World Patient Impact translates to patients unable to find accurate provider information, delayed or disrupted care from directory errors, and member frustration that drives plan switching..
V. Modern Approaches to Provider Data Management
Traditional Approach: Manual and Batch Processing relies on quarterly or annual directory update cycles, spreadsheet-based data collection, manual verification phone calls and surveys, and batch file transfers between systems. The result: slow, error-prone, labor-intensive processes that cannot keep pace with regulatory requirements or member expectations.
API-Driven Infrastructure: The Modern Standard enables real-time data exchange between systems, automated verification and validation, single integration to access multiple carrier networks, and continuous compliance monitoring. IdeonSelect exemplifies this modern standard, providing normalized provider data via unified API that eliminates the need to build and maintain individual carrier integrations.
Benefits of API-First Architecture:
- Speed: 4-8 weeks implementation vs. 12-18 months for custom builds
- Accuracy: Automated quality control and normalization eliminate manual errors
- Compliance: Built-in regulatory update automation keeps pace with CMS, NSA, and state requirements
- Scalability: Handle enrollment surges without manual intervention
- Cost efficiency: Subscription model replaces expense of building and maintaining infrastructure
Cloud-based centralization provides single source of truth with real-time updates and enterprise-grade security (SOC 2 Type II, HIPAA compliance). API-driven PDM connects seamlessly to HRIS, payroll, benefits platforms, and claims processing systems.
VI. Implementing Effective PDM
Assessment Phase evaluates current data quality and accuracy rates, identifies system fragmentation and integration gaps, documents compliance requirements and deadlines, and calculates total cost of ownership for existing manual processes.
Strategic Decision: Build vs. API Infrastructure
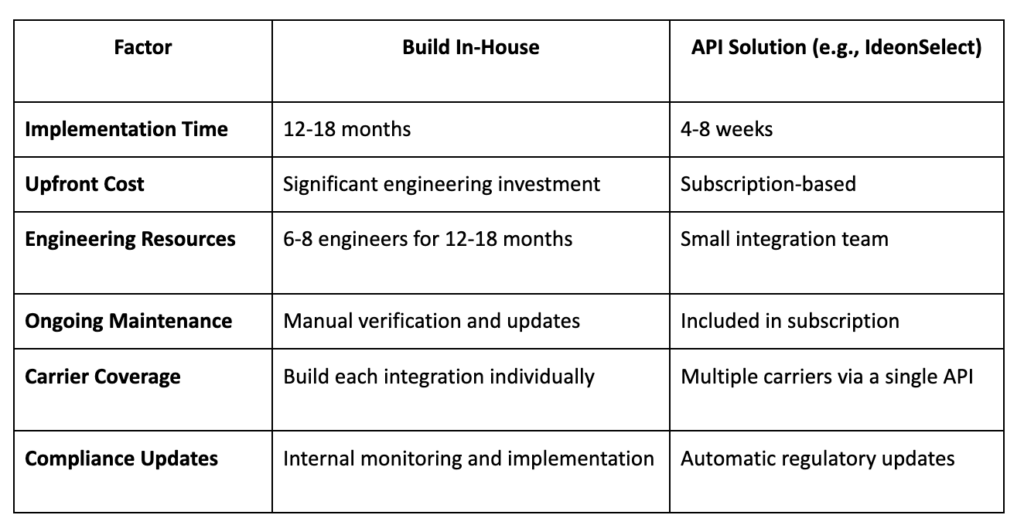
Implementation Best Practices include establishing data governance frameworks with clear ownership, defining quality metrics and monitoring processes, planning phased rollouts prioritizing compliance requirements, and monitoring member satisfaction alongside directory accuracy metrics.
VII. The Future of PDM
Regulatory Landscape Evolution continues with the CMS Plan Finder mandate (2027) requiring Medicare Advantage plans to publish directories to a centralized federal resource. State-level enforcement is intensifying with increasing penalties for directory inaccuracies.
Technology Acceleration makes API-first infrastructure the industry standard as real-time verification replaces quarterly batch updates. AI-powered data validation and automated compliance reporting add additional accuracy layers.
Member Expectations Rising demand real-time accuracy, comprehensive provider details, and integration with telehealth and digital care navigation that legacy systems cannot support.
Infrastructure as Competitive Advantage: Organizations leveraging modern API-driven PDM launch products faster, maintain compliance automatically, and deliver superior member experiences—while competitors struggle with 12-18 month build timelines and manual verification burdens.
Conclusion: Provider Data Management as Strategic Infrastructure
Provider data management has become strategic infrastructure determining competitive position. The requirements are clear: CMS 90-day verification cycles, No Surprises Act 1-day response times, Medicaid 30-day updates. Member expectations are equally demanding: 62% seek precise provider data, and over 33% will switch plans for better digital capabilities.
Organizations face a strategic choice. Build complex infrastructure internally—12-18 months development, significant engineering investment, ongoing operational costs for manual verification and compliance monitoring. Or integrate API solutions like IdeonSelect—4-8 weeks implementation, subscription-based pricing, automatic compliance updates included.
Modern API-driven infrastructure enables rapid implementation while ensuring accuracy, compliance, and scalability—freeing organizations to focus on product differentiation rather than data plumbing.
Explore Ideon's IdeonSelect for Provider Data Management
Ready to take the next step? See how Ideon works.
